August 2021
Global consortium representing 27 institutions compared mortality in the previous five years to deaths between January and August 2020. They found that some countries showed excess all-cause mortality, while other nations had minimal or even decreased excess mortality.
Since the earliest weeks following the emergence of SARS-CoV-2, it has been a challenge to understand the impact of the pandemic on mortality. COVID-19 death counts do not account for limited testing, upended healthcare systems, and deaths stemming from restriction measures. In short, countries worldwide are lacking an accurate picture of the direct and indirect mortality burden from COVID-19.
The University of Nicosia (UNIC), its Medical School, and research collaborators took note of this international problem and devised the sort of global-scale project needed to address it. They launched the COVID-19 Mortality (C-MOR) Consortium which welcomed countries from around the world and focused on measuring excess mortality. This type of analysis would enable the researchers to assess all-cause deaths during the pandemic along with all-cause deaths during the same period in previous years. As such, the Consortium could more accurately measure how the pandemic affected mortality in countries across the globe.
The consortium’s first step was to assemble a globally representative team. What started with just one university has since grown to 58 institutions across 6 continents and 52 countries. Consortium partners in 22 of these countries were able to navigate through shared challenges of collecting and analysing five years of mortality data from largely primary sources. Their hard work and collaboration paid off with a truly global dataset focused on excess mortality from the inception of the pandemic through to August 2020. This work was published this week in the International Journal of Epidemiology by the Oxford University Press (Excess all-cause mortality and COVID-19 related mortality: a temporal analysis in 22 countries, from January until August 2020).
“As emerging and re-emerging infectious diseases become more common, our results provide valuable lessons on the impact epidemics can have on populations and also offer insight on what can be done to mitigate this impact”, remarked Dr. Christiana Demetriou, the Consortium’s principal investigator.
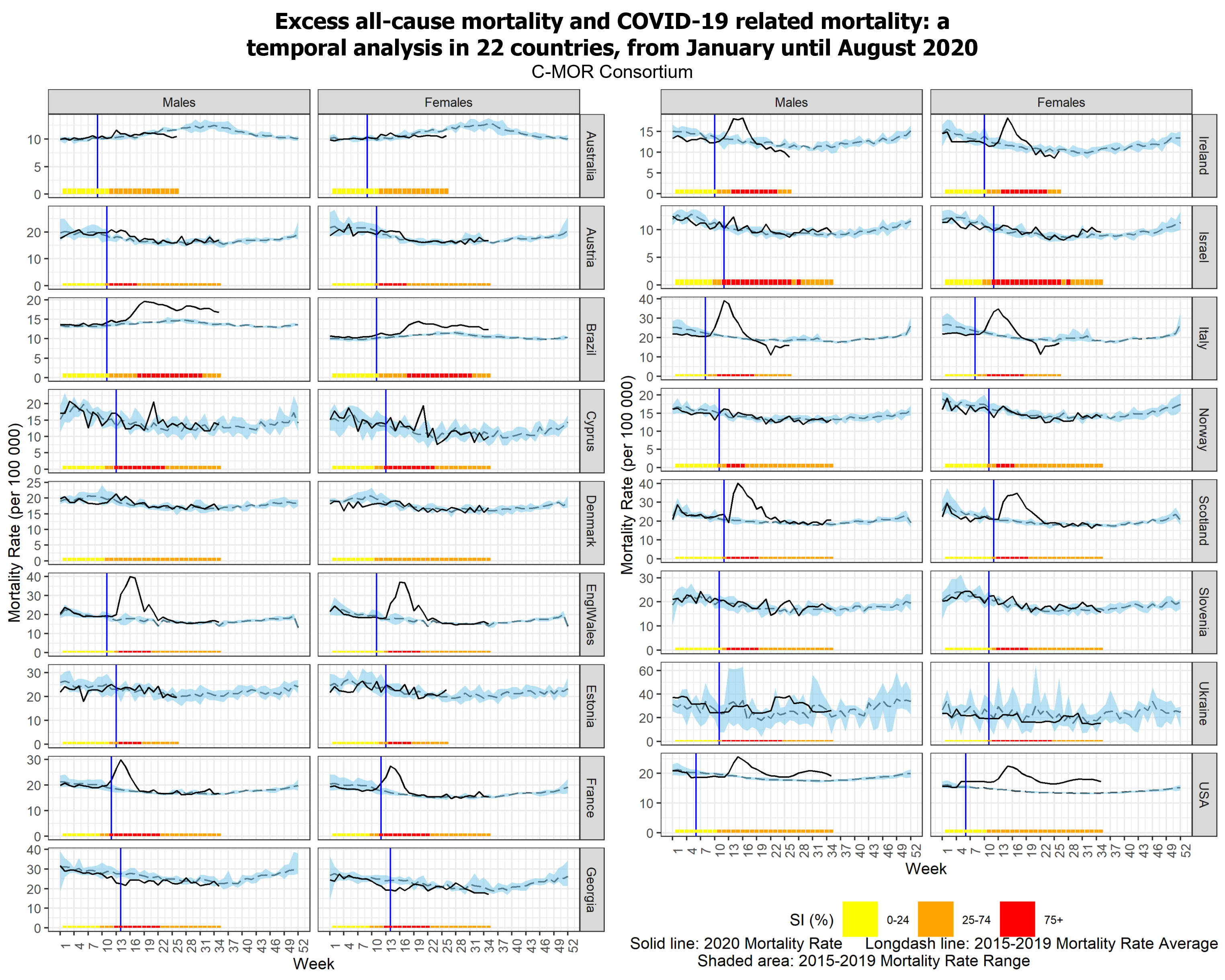
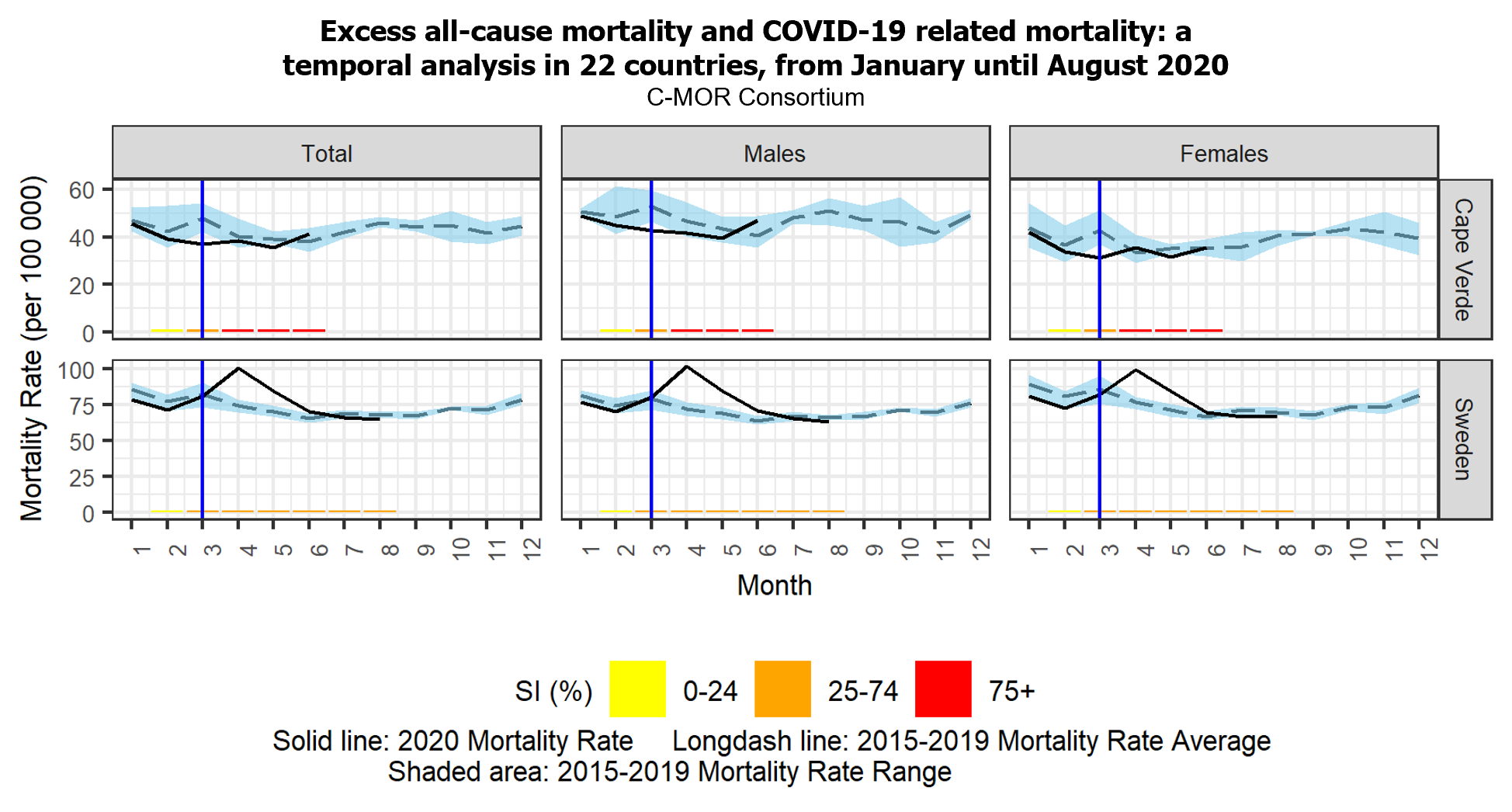
The study shows that some of the 22 countries had increased all-cause excess mortality (Brazil, England, France, Italy, Northern Ireland, Scotland, Spain, Sweden, the USA, and Wales), some had insignificant excess mortality (Austria, Cape Verde, Colombia, Cyprus, Estonia, Israel, Norway, Slovenia, and Ukraine), and some even had reduced excess mortality (Australia, Denmark, and Georgia).
For five of these countries (Cape Verde, Cyprus, Georgia, Slovenia, and Ukraine) this is the first published analysis on excess mortality. Furthermore, this is one of the few studies to examine excess sex-specific mortality. The researchers found that females drove excess deaths in Ireland, while only males in Israel, Ukraine, and Italy had increased mortality. Another unique variable assessed in this study was governmental restriction measures. The authors note that the countries with increased excess mortality tended to have limited or delayed control measures, and vice-versa. Additionally, the study describes that patterns of mortality found in the cases of Australia, Cape Verde, and Colombia are likely influenced by the timing of the pandemic in these countries, with their more southern latitudes.
These results represent one of the largest and most expansive studies of mortality from the pandemic that predominantly utilized national and primary sources, as opposed to publicly available datasets. Researchers with on-the-ground experience collected the data for each of their respective countries. While the valuable lessons in this study make their way to policy-makers and healthcare professionals, the Consortium remains hard at work aiding in the response to this pandemic and future ones. In this vein, it is expanding its research questions to include morbidity, considering phenomena like long-covid, long-term effects of covid following recovery, along with potential-years-of-life-lost from COVID-19.
Dr. Demetriou, who is also an Assistant Professor of Epidemiology and Public Health at UNIC Medical School, noted, “as we face this politicized pandemic, the consortium is actively collecting accurate and timely surveillance data. We will not only continue to monitor excess deaths but will also begin to study the morbidity burden from COVID-19. These analyses will help us to better understand and minimize the multi-dimensional health effects of the virus”.
To find out more about C-MOR and how to get involved please visit www.unic.ac.cy/coronavirus/mortality/ or email the C-MOR project coordinator at [email protected]. You can access the full list of the Consortium partners that contributed to this study here.